Clinic Locations
Jacksonville/Southside
St. Johns
Ponte Vedra
P: (904) 996-6922
F: (904) 996-6923
info@premierptjax.com
Physical Therapy in Jacksonville
Expert Care and
Lasting Results
Personalized therapy where your well-being comes first.
5-Star Google Rating
We are proud to have a 5-star Google rating! This demonstrates our commitment to excellent service and hopefully builds trust with new customers!
Best of Ponte Vedra
We are the Best of Ponte Vedra 2023 winners! We could not have done this without the help of our wonderful clients!
Over 150 Five Star Reviews
We are proud to have earned the trust of over 150 people who left us a 5-star review. Our team continues to provide the best physical therapy!
Top Rated Physical Therapists in Jacksonville
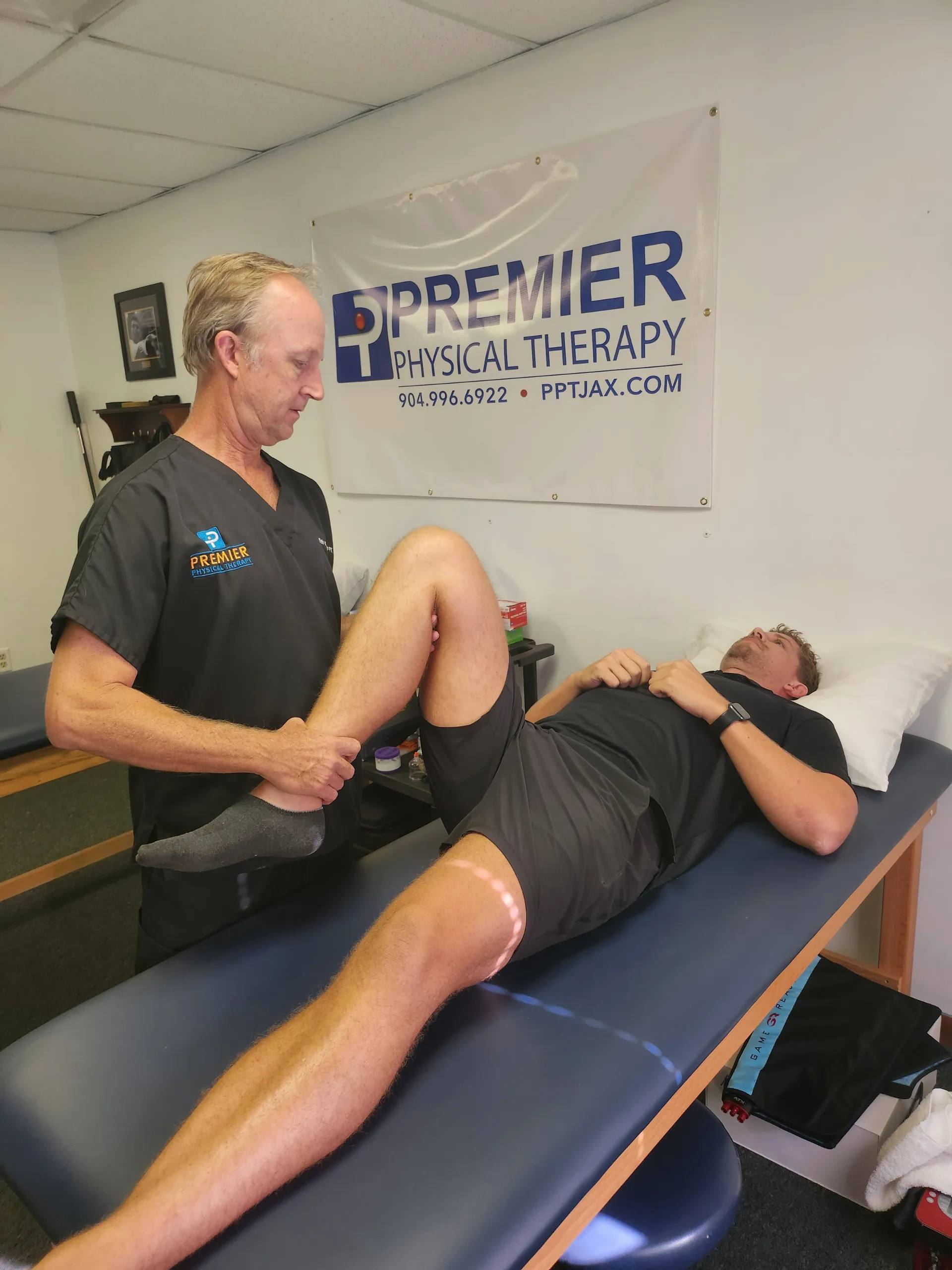
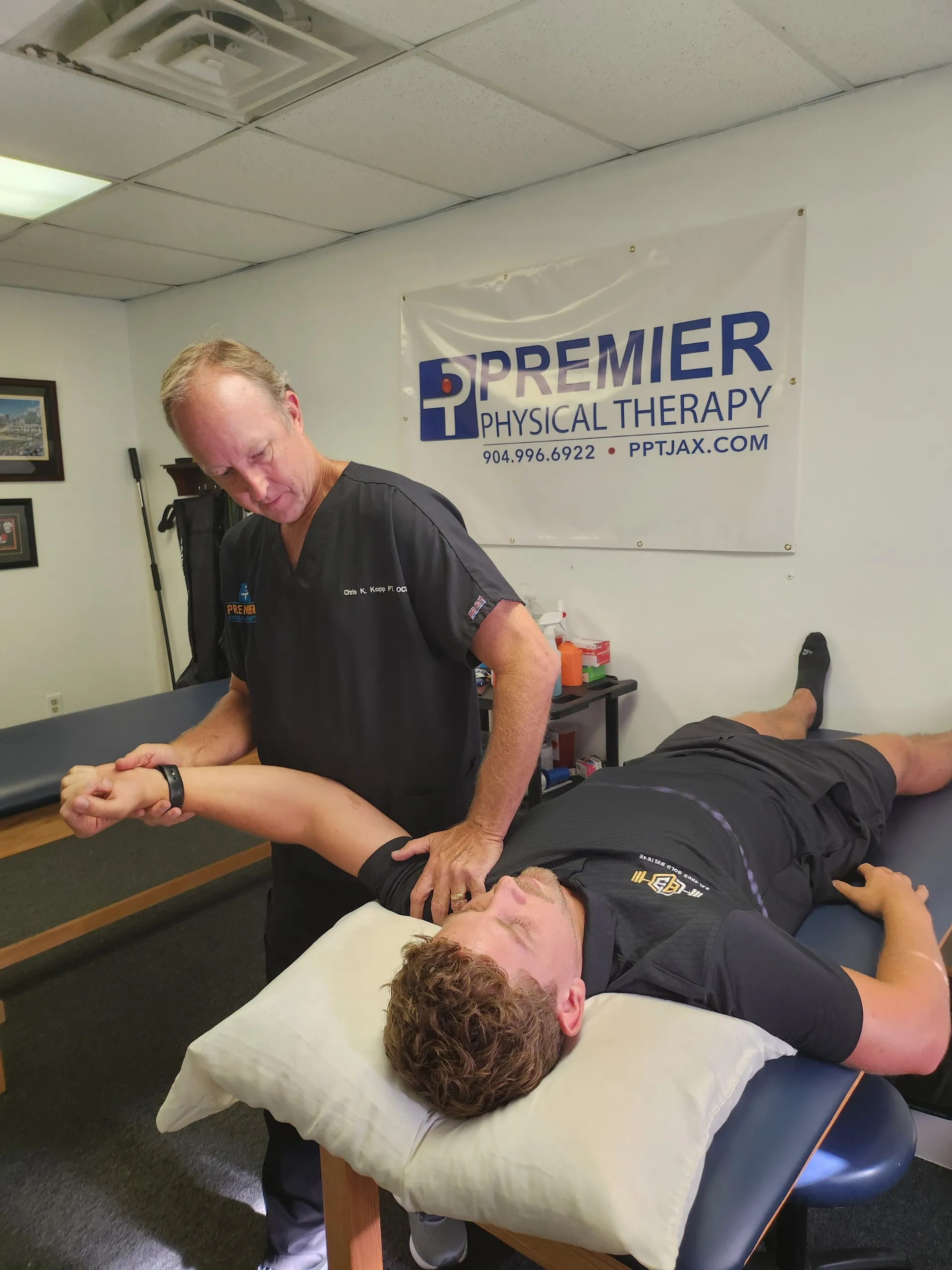
If you're looking for a physical therapist, we have the perfect opportunity for you. Every member of our team has received professional training and is licensed. We can provide dry needling and therapy for any injury or emergency. You can trust our reliable solutions and professional service to ensure that your body is well-maintained.
Our physical therapists are proud to create individualized and personal physical therapy treatment plans that are unique to each individual. They also provide extensive education about how to improve one's health and prevent future injuries.
Personalized Care from Our Team
There are no two people exactly the same. Therefore, injuries can be different even though they may affect the same body part. Our expert medical team will evaluate your condition and create a customized treatment plan that will get you back on track to being your best. Our staff will guide you through each visit with personalized attention and dedication.
Live Pain Free in Jacksonville
Our team understands that you want to live an active lifestyle that is comfortable and capable. Your body must work in order to achieve that. You are experiencing pain, injury or weakness, which can make you feel confused and frustrated.
We believe that you deserve a body that is fully functional. We know what it is like to be injured,which has led to our success in helping thousands of people get back to their active lives.
This is how we do it:
- Tell us your story
- Get your customized plan.
- Start feeling better.
- Conquer your goals
Our Physical Therapy Programs
Testimonials

“D H”
5 star experience here every time. Chris and his team (primarily Kurtis, in my case) rehabbed me through three separate injuries over the past couple years with great success each time. This group has a very knowledgeable staff that takes the time to do it right…
“Gino Federico”
From my first interaction with Katrina, to my last appointment with Taylor, Premier Physical Therapy has been Phenomenal. I’m very satisfied with their services and helping me get back to a healthy normal. My only regret is that I didn’t come here sooner after my initial injury. Highly recommend!
“Dan Croft”
These guys are the best – if you want results you can’t do better than Chris and his team. During my post-op rehab, I’ve made more progress in two weeks with Premier than my previous PT big-system provider achieved in two months. I look forward to meeting my goals soon, thanks to Chris, Beverly, Kurtis and the rest of the Premier PT team. Thanks!
“Marissa Alex”
Each and every person at Premier Physical Therapy are caring and concerned individuals, as well as knowledgeable in their field. Chris and his staff are friendly and fun, moreover they look forward to working with you and building on your progress. My husband and I both consider Chris the best PT in handling your physical needs while helping you achieve your goals.
Our Proven 4-Phase Recovery Program


Pain
It can be frustrating and overwhelming when you’re in pain and don’t know where to turn for help. Our physical therapy experts will work with you one-on-one to identify the root cause of your pain and create a personalized treatment plan that will reduce your pain quickly. We’ll also provide you with helpful resources like exercises and pain reduction tips so you can continue to progress even after leaving our clinic. On average our patients see a significant reduction in pain in 6 visits or less.

Prime
We all know that reducing pain is important, but sometimes it’s hard to stay motivated after the initial relief. It can be tough to keep up the momentum after your pain has subsided. You may feel like you’re stuck in a rut and don’t know how to get moving again. During Phase II, we help you regain your mobility, flexibility, and strength so you can continue on your path to success. With our help, you’ll be primed for future performance and able to prevent injury.
Perform
You’ve been sidelined by an injury and you’re eager to get back to your old self as soon as possible. It’s frustrating when you’re injured and can’t do the things you love. Sitting on the sidelines is hard, especially when everyone else seems to be moving on without you. That’s where our physical therapists come in. We’ll help you rehab your injury so that you can get back to your old self as quickly as possible. With our personalized treatment plans and experienced therapists, we’ll have you feeling like yourself again in no time.
Prevent
You’ve just suffered an injury and the last thing you want to do is go through the pain again. It’s normal to feel concerned that the injury will occur again. In fact, most people worry about this very thing. That’s why our physical therapists make sure that you are equipped with the tools needed to prevent any future injury. We’ll help you recover quickly and safely so that you can get back to your life as soon as possible.
See the difference! Request a physical therapy session today!
Success Stories & Testimonials

Meet Our Team

Dr. Chris Kopp
PT, DPT, OCS, CMPT, TPI CERT.
CLINICAL DIRECTOR
Dr. Mark Kosier
DPT, PT, FOMPT, RCMT, CERT DN, TPI CERT.
Dr. Lisa Spink
PT, DPT, TPI CERT.
Treatments


Alter-G
Your Subtitle Goes Here
The Alter-G Anti-Gravity Treadmill is a game-changer in the world of sports rehabilitation and training. It utilizes innovative Differential Air Pressure (DAP) technology to reduce the impact of gravity on your body,
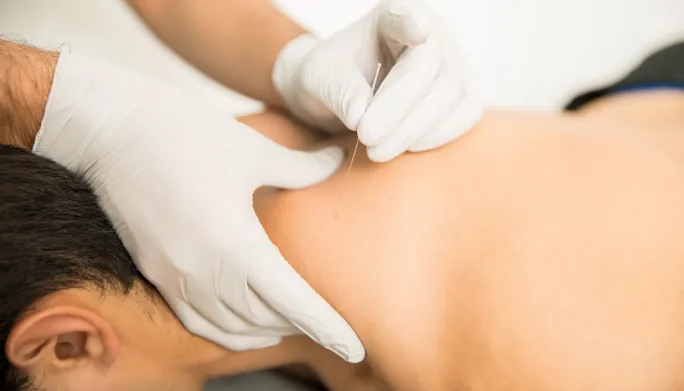
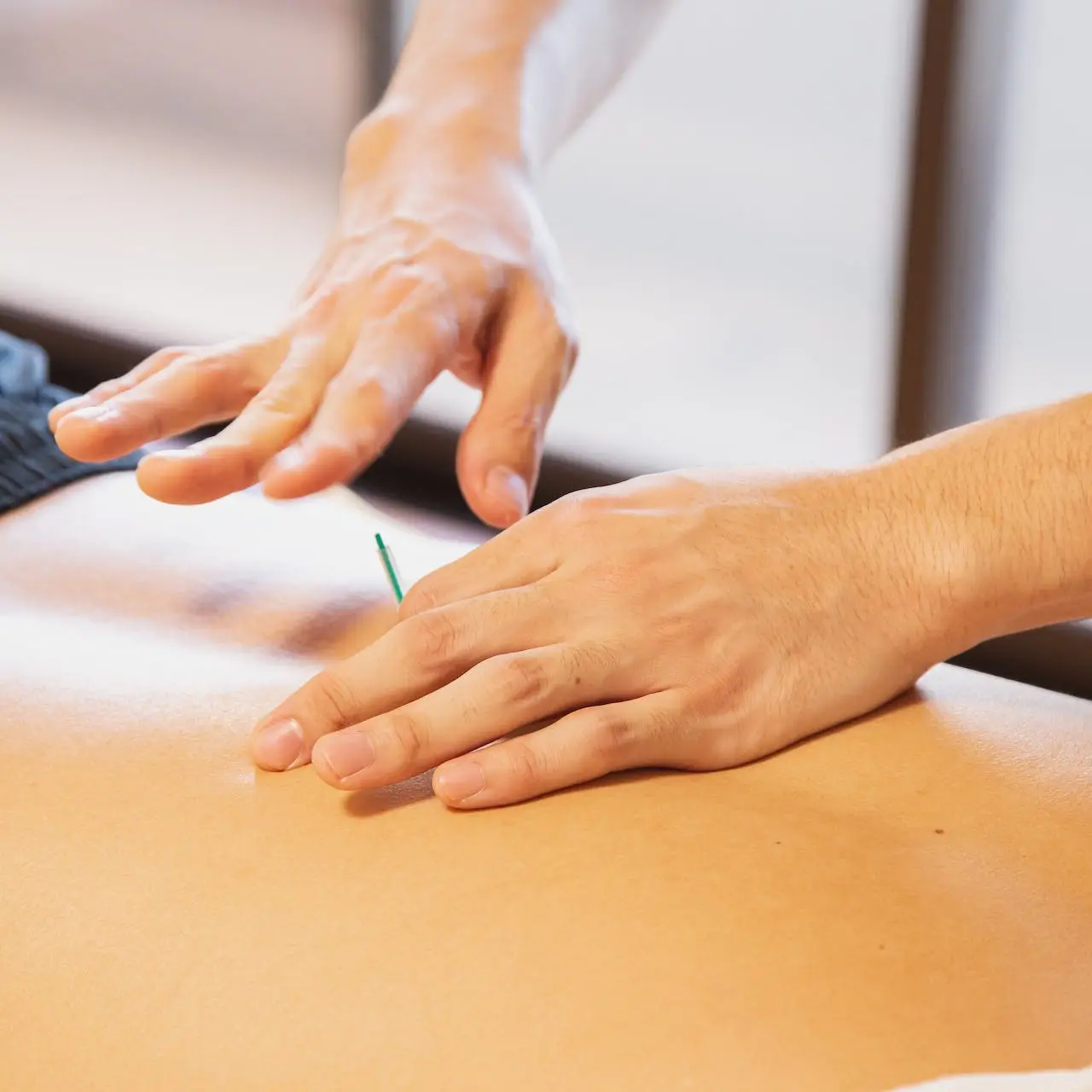
Dry Needling
Your Subtitle Goes Here
If unrelenting muscle tension, restricted mobility from past injuries, or unresolved neurological and movement dysfunction has you struggling to perform basic tasks pain-free…

Golf Rehab
Your Subtitle Goes Here
Based on research of the top PGA pros compared to amateur golfers, specific musculoskeletal limitations prevent golfers from reaching their full potential. Certain physical limitations lead to chronic injuries that will take you out of the game and lessons..

Physical Therapy
Your Subtitle Goes Here
From weekend warriors dealing with nagging pain to aging adults hoping to remain independent, patients choose Premier Physical Therapy for customized physical therapy delivered with compassion…

Sports Rehab
Your Subtitle Goes Here
Is your game stalled by injury or just not measuring up anymore due to mobility restrictions or strength deficits? Let Premier Physical Therapy’s sports rehabilitation team help you recapture your physical prowess and competitive edge.

Cupping
Your Subtitle Goes Here
If chronic injuries, inflammation, or muscular tension has you feeling less than your best, exploring cupping therapy with Premier Physical Therapy can help get you back on track. This ancient healing art uses targeted suction to reduce aches…

Geriatric Physical Therapy
Your Subtitle Goes Here
The aging process can gradually lead to more aches, pains, reduced strength, balance and coordination issues impeding daily functioning and safety for older adults. Until immobility and isolation seem inevitable.

Pediatric Orthopedic Rehab
Your Subtitle Goes Here
If you are a youth, collegiate, elite, or professional athlete, when you are injured, you need a physical therapist with experience rehabilitating sports-related injuries. Athletes place higher demands on the muscles…

Remote Therapeutic Monitoring
Your Subtitle Goes Here
Remote Therapeutic Monitoring is like having your physical therapist right in your pocket. We use the latest technology to check on how you’re doing with your exercises, pain, and function without you having to step foot outside your home.

TPI
Your Subtitle Goes Here
TPI programs focus on the physical and biomechanical aspects of the golf swing, helping golfers develop a more efficient and effective swing. Through a combination of exercises, drills, and personalized coaching, our TPI programs help golfers improve their balance..


Alter-G
Your Subtitle Goes Here
The Alter-G Anti-Gravity Treadmill is a game-changer in the world of sports rehabilitation and training. It utilizes innovative Differential Air Pressure (DAP) technology to reduce the impact of gravity on your body,


Cupping
Your Subtitle Goes Here
f chronic injuries, inflammation, or muscular tension has you feeling less than your best, exploring cupping therapy with Premier Physical Therapy can help get you back on track.
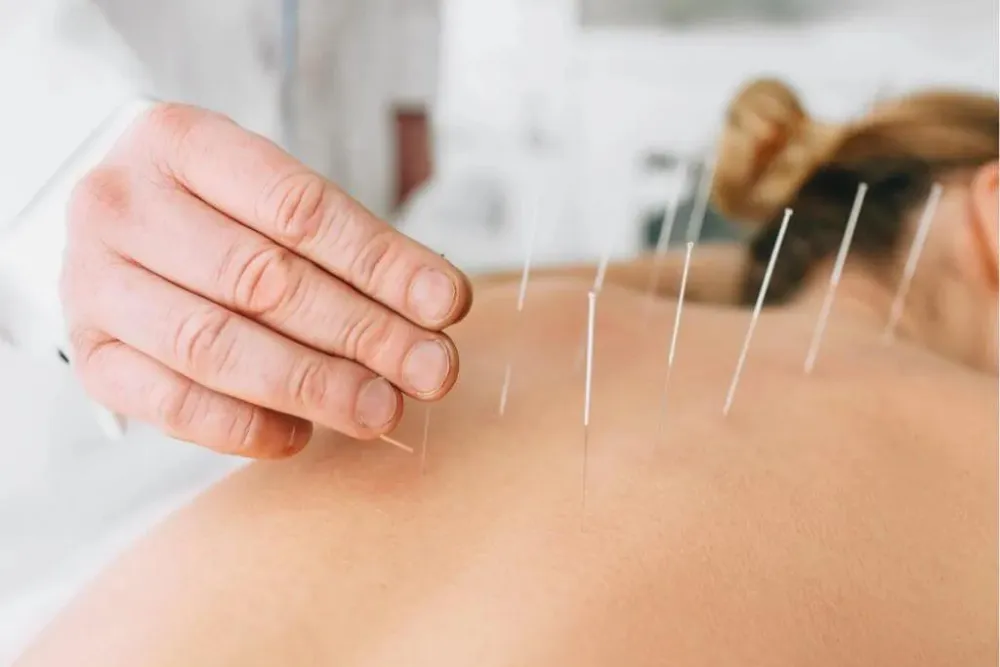

Dry Needling
Your Subtitle Goes Here
If unrelenting muscle tension, restricted mobility from past injuries, or unresolved neurological and movement dysfunction has you struggling to perform basic tasks pain-free,


Geriatric Physical Therapy
Your Subtitle Goes Here
The aging process can gradually lead to more aches, pains, reduced strength, balance and coordination issues impeding daily functioning and safety for older adults.


Golf Rehab
Your Subtitle Goes Here
Based on research of the top PGA pros compared to amateur golfers, specific musculoskeletal limitations prevent golfers from reaching their full potential.


Pediatric Orthopedic Rehab
Your Subtitle Goes Here
If you are a youth, collegiate, elite, or professional athlete, when you are injured, you need a physical therapist with experience rehabilitating sports-related injuries.


Physical Therapy
Your Subtitle Goes Here
From weekend warriors dealing with nagging pain to aging adults hoping to remain independent, patients choose Premier Physical Therapy for customized physical therapy delivered with compassion.


Remote Therapeutic Monitoring
Your Subtitle Goes Here
Remote Therapeutic Monitoring is like having your physical therapist right in your pocket. We use the latest technology to check on how you’re doing with your exercises, pain, and function without you having to step foot outside your home.


Sports Rehab
Your Subtitle Goes Here
Is your game stalled by injury or just not measuring up anymore due to mobility restrictions or strength deficits? Let Premier Physical Therapy’s sports rehabilitation team help you recapture your physical prowess and competitive edge.


TPI
Your Subtitle Goes Here
TPI programs focus on the physical and biomechanical aspects of the golf swing, helping golfers develop a more efficient and effective swing. Through a combination of exercises..
Stop Letting Pain Get In The Way
Premier Physical Therapy Treats All Of These Conditions & More!

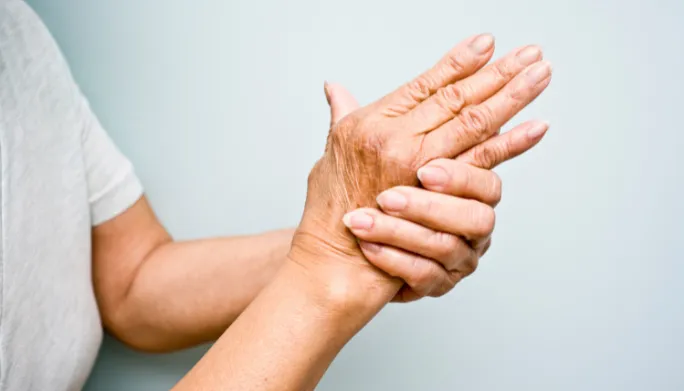
Arthritis

Back Pain

Gait Disorders

Chronic Pain

Dizziness

Hand Pain
Testimonials

Frequently Asked Questions

What should I expect during physical therapy sessions?
Physical therapy sessions typically involve an assessment of your condition, manual techniques to improve mobility and flexibility, individualized exercises and activities to help you reach your goals, education on how to prevent further injury or pain, and instruction on proper posture, body mechanics and other lifestyle changes.
Do I need a referral from my doctor before attending Physical Therapy?
Florida is a “direct access state.” This means you are allowed to go directly to a physical therapist without a physician’s referral first and receive treatment for 30 days.
What do I need to wear or bring with me?
You should dress in comfortable, loose clothing that allows you to move easily and doesn’t restrict circulation. Depending on your condition, your physical therapist may also recommend special shoes or a brace. You should also bring any paperwork related to your medical history, including x-rays, ultrasounds, and doctor’s notes.
Is there anything I can do before my appointment to prepare?
Yes! Make sure you arrive for your session well-rested so that you can give it your full attention and energy. It is also helpful if you keep track of how much pain medication (if any) you take prior to the appointment so that the physical therapist can adjust the intensity of treatment accordingly.
How long will my physical therapy sessions last?
Sessions typically last 30-60 minutes depending on your condition and the types of techniques used. Your physical therapist will give you an estimate when you first arrive for your appointment.
Are there any exercises I can do at home between appointments to help improve my condition?
Yes! Your physical therapist may provide specific exercise recommendations for you to try in between visits, which will help speed up your recovery and progress faster toward reaching your goals. It’s important to follow these carefully and always check with your PT before starting a new exercise program if you have any questions or concerns.
What if I have questions after my physical therapy session?
Your physical therapist should be available to answer any questions or concerns you may have about your treatment plan before and after each visit. You can also contact the clinic directly for further assistance. We want you to get the most out of every session!
Will insurance cover my physical therapy?
It depends on your insurance plan. Most plans cover some or all of the costs associated with physical therapy, but you should check with your provider to determine coverage and any associated fees.
How often will I need to attend physical therapy sessions?
The frequency of visits will depend on your individual goals and condition, but typically it is recommended that patients attend 2-3 times per week for a minimum of 4-6 weeks in order to maximize results. Your therapist will provide more details during your initial appointment.
How long will it take for me to see results?
Every person’s situation is unique; therefore the amount of time needed to reach goals varies. With commitment and dedication from both you and your physical therapist, you can expect to start seeing results within a few weeks. The more positive lifestyle changes you make, the faster your progress will be!
Will my physical therapist be able to answer any questions I have about my condition?
Yes! Your physical therapist should be available to discuss any concerns or questions you have regarding your condition or treatment plan. Don’t hesitate to bring up any issues that may arise during the course of therapy.
What if I feel too much pain during a session?
If at any time during your physical therapy session you experience increased pain, it’s important to let your therapist know so they can adjust the intensity or technique as necessary. Your therapist will work with you to make sure that treatment is comfortable and effective for you.
How will I know when I no longer need physical therapy?
Your physical therapist should be able to provide guidance on when it is appropriate to stop attending physical therapy sessions based on your progress, goals, and overall health status. It’s important to listen to your therapist and continue with treatment until they feel you are ready to move on.